Left To Right Shunt Lesions: Patent Ductus Arteriosus (PDA) & Eisenmenger Syndrome
PDA
Clinical Cardiology
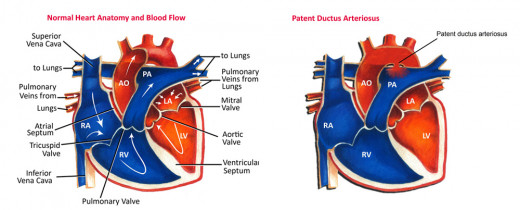
Patent Ductus Arteriosus
This is seen more commonly in children. Embryologically, the ductus arteriosus is the persistent left sixth aortic arch. In the fetus, it allows the egress of blood pumped from the right ventricle into the pulmonary trunk to the descending aorta bypassing the lungs which are non-functional. Normally, as the lungs get aerated after birth, functional closure of the ductus occurs in 24 hours and anatomical closure within 1-2 weeks after delivery. Patency of the ductus after birth results in the flow of blood from the aorta to the pulmonary artery since the pulmonary artery pressure is lower.
The aortic end of the ductus lies beyond the origin of the left subclavian artery and the pulmonary trunk, in the early stages of the disease, blood from the aorta flows to the pulmonary artery throughout systole and diastole. When pulmonary hypertension develops, this blood flow diminishes, initially the diastolic flow. The blood flow may be reversed when Eisenmenger syndrome develops.
Patent ductus arteriosus is more common in females and in premature infants. It may occur as an isolated lesion or as part of a complex anomaly with other congenital heart diseases. Maternal rubella is associated with increased incidence of PDA in the child. Clinical features depend upon the amount of left to right shunt through the ductus.
Clinical features
The pulse may be collapsing in character, there is left ventricular type of cardiac enlargement. Cases with Pulmonary hypertension may reveal left parasternal heave. In the vast majority of cases, a continuous thrill may be felt over the left second intercostals space outside the sterna border. The most characteristic auscultatory finding is the presence of a continuous machinery type of murmur, audible most loudly over the left upper sterna border. The murmur is louder during systole and less so during diastole. The systolic phase is interrupted by multiple systolic clicks. Less commonly, large shunts may be accompanied by left ventricular third heart sound followed by a decrescendo mid-diastolic murmur best heard over the apex beat. This indicates large blood flow across the mitral valve. The second heart sound is usually immersed in the murmur. In cases with pulmonary hypertension, the pulmonic component becomes louder and well-heard.
Course and prognosis
Mild cases do not impair cardiac function and they may remain asymptomatic. Large ductus may present with congestive heart failure in infancy. Those cases which recover from heart failure may develop pulmonary hypertension later in life. Large left to right shunt leads to enlargement of left atrium, left ventricle, aorta and pulmonary artery.
Complications
Cardiac failure, infective endocarditis, paradoxical embolism and Eisenmenger syndrome may complicate PDA.
Treatment
Patent ductus arteriosus is corrected by surgical closure preferably during childhood itself. During the neonatal period, medical closure of the ductus can be attempted by the administration of indomethacin in a dose of 0.05 to 0.1mg/kg body weight. Indomethacin exerts this effect by inhibiting prostaglandin, which is responsible for maintaining patency of the ductus.
Diagnostic Of Eisenmenger Syndrome

Eisenmenger syndrome
Pulmonary hypertension may develop at variable periods of time in congenital heart disease with initial left to right shunt. When severe pulmonary hypertension develops, the volume of left to right shunt diminishes. As the pulmonary artery pressure increases, the shunt becomes bidirectional and finally the flow is only from right to left. When the right to left shunt leads on to a clinical picture of cyanosis, the condition is designated as Eisenmenger Syndrome. The common congenital anomalies which cause Eisenmenger syndrome are ventricular septal defect, patent ductus arteriosus, and atrial septal defect. The VSD and PDA give rise to Eisenmenger syndrome in childhood itself whereas ASD gives rise to this picture usually after the third decade of life.
Clinical features
The clinical hallmark of Eisenmenger syndrome is the combination of central cyanosis, digital clubbing and pulmonary hypertension. In some cases, the central cyanosis may be mild and not obvious at rest. Exercise unmasks the cyanosis in such cases. In PDA with Eisenmenger syndrome, the cyanosis and clubbing are present only in the lower limbs (called differential cyanosis and clubbing) because the patent ductus joins the aorta after the origin of the left subcalvian artery so that the desaturated blood goes only to the lower limbs.
Course and prognosis
Once Eisenmenger syndrome develops, the symptoms related to left to right shunt disappear. At this stage, easy fatigability and tiredness dominate the clinical picture. Once congestive heart failure sets in, steady deterioration occurs culminating in death within 3-5 years.
© 2014 Funom Theophilus Makama